In This Issue
Message From Jim Bagian, CHEPS Director
Alumni Spotlight: Joe East
CHEPS at INFORMS
Faculty Spotlight: Richard Hughes
Block Scheduling
Recent News
Upcoming Events
Where In The World Is CHEPS?
Message From Jim Bagian, CHEPS Director
Welcome to the April 2017 issue of CHEPS Pulse. It’s a pleasure to share some of the people and projects that make CHEPS the outstanding center that it is.
Joe East graduated in the very first class of our HEPS master’s concentration. He’s now at Maine Medical as where he holds the title of Manager, Patient Access and Flow. He shares his views on the intersection of engineering and healthcare as well as some tips he’s learned through his time at CHEPS and beyond that I believe will be valuable to all readers.
Richard Hughes has been an affiliate of CHEPS since its inception. His work today focuses on quality improvement in hip and knee replacement (arthroplasty). Along with Dr. Brian Hallstrom, M.D., he is Co-Director of the Michigan Arthroplasty Registry Collaborative Quality Initiative (MARCQI).
As always, there are many exciting and innovative research activities taking place at CHEPS. Below, you’ll get an in-depth look at our Block Scheduling project. This project grew from building the daily resident shift schedules for C.S. Mott’s Pediatric Emergency Department to scheduling for Pediatrics, Internal Medicine, Combined Medicine-Pediatrics, and more than a dozen programs in the Department of Surgery and we foresee further growth in the future. You’ll also get a glimpse of a few more of the projects happening at CHEPS with our video showcasing a few of our students who attended the 2016 INFORMS Annual Meeting in Nashville.
I hope you enjoy learning a little bit more about what’s going on here at CHEPS in this newsletter. If you have suggestions about what you’d like to see us feature in future issues, please get in touch at [email protected]. You can also follow us on Twitter to get a glimpse of day to day life in the Center at @UofMCHEPS.
Be on the lookout for more news from us throughout the year. I look forward to keeping in touch with all of you to keep you up to date.
James Bagian MD, PE
CHEPS Director
Alumni Spotlight: Joe East
Joe East graduated from The University of Michigan in 2014 with a joint masters degree in Industrial and Operations Engineering (IOE) and Health Management and Policy. He was also a member of the first class of students at the Center for Healthcare Engineering and Patient Safety (CHEPS) to add a concentration in Healthcare Engineering and Patient Safety (HEPS) to his IOE masters degree.
Joe saw the combination of these degrees along with his HEPS concentration as a unique opportunity. “We are in a great time of opportunity in these two fields: the tools and analytical problem solving developed in IOE provide new approaches to enhance people’s health and improve decision making in healthcare and public health,” he explained. Although the work needed to complete the degrees simultaneously was immense, Joe believes that the benefits outweighed the costs. He states that “completing both programs gave the benefit to take the ideas in one and apply to the other which has been invaluable in the first years after graduating.”
After graduation, Joe spent some time hiking in Patagonia before starting at Maine Medical. He began his time at Maine Medical as an Administrative Fellow and now holds the title of Manager, Patient Access and Flow. With nurse, physician, and administrative partnerships across the hospital, he helps lead some of their major initiatives to better utilize existing inpatient capacity at the 637 bed, academic medical center in Portland, Maine. He also co-manages the bed placement and patient transfer center.
Over his past two years working at Maine Medical, Joe has come up with three tips that he says have helped him daily:
1. “Focus on shared organizational values. Most organizations have them defined, great ones live them out in decisions made every day. In businesses that often have thousands of staff seeking to serve thousands more patients, there are many competing priorities and urgency of different perspectives. Common values, truly embraced, provide a common direction.”
2. “Always seek to learn from others. In an industry that’s fantastically interdisciplinary, there are dozens of stakeholders involved in almost every situation. Learning and teaching others well helps to navigate some of the nuances of our work more smoothly.”
3. “Data and stories are key. Analytical and statistical tools help provide a common language to build understanding and guide the right path to take. Experiences are not to be undervalued, though. They reach close to the patients and care teams we seek to serve and often are what motivate others to embrace the advancements we seek to make together.”
Joe doesn’t allow his life to be all work. He’s spent much time traveling, last year to South Africa and this year to Japan. Additionally, in the coming year, he’ll be heading back to Michigan to marry his fiancée, Nicole. All of us at CHEPS are looking forward to seeing what this next chapter in Joe’s life holds for him and we wish him the best!
Video: CHEPS at INFORMS
Several CHEPS students attended the 2016 INFORMS Conference in Nashville, Tennessee from November 13 – 16, 2016. They enjoyed ample opportunities to collaborate and share research and insights.
This video highlights some of the students who attended the conference.
Faculty Spotlight: Richard Hughes
Richard Hughes received his PhD in Industrial and Operations Engineering (IOE) at the University of Michigan in 1991. In 1998 he returned to the University of Michigan as a faculty member in the Department of Orthopaedic Surgery. In the interim, he completed a post-doctoral fellowship at the Mayo Clinic and worked at the Washington State Department of Labor and Industries as an ergonomist as well as the federal Centers for Disease Control and Prevention as a human factors engineer.
He chose to join a clinical department upon returning to academia. He says of the choice, “I feel that being in a clinical department gives me a much better understanding of clinical problems than being in an engineering school would. Living – so to speak – in the clinical world gives me a more solid sense of what kinds of problems are important to solve.” Since 1998 he has obtained appointments in IOE and Biomedical Engineering as well. He became a CHEPS associate when the center was founded.
His work today focuses on quality improvement in hip and knee replacement (arthroplasty). Along with Dr. Brian Hallstrom, M.D., Dr. Hughes is Co-Director of the Michigan Arthroplasty Registry Collaborative Quality Initiative (MARCQI). MARCQI is a network of 59 hospitals across Michigan that work together to improve the quality of care for hip and knee arthroplasty patients by sharing best practices.
While Dr. Hughes has been successful as an academic, publishing 98 papers in clinical and engineering peer-reviewed journals, he feels dissatisfied with the disconnect between academia and the larger world of healthcare delivery. “I miss working in the public sector doing applied work that helps many people, which is one reason that I joined with Brian Hallstrom to create MARCQI. It allows me to use the analytical tools and methods of industrial engineering to make meaningful changes in health care across the state,” he says. “For example, MARCQI has reduced the rate of transfusion in hip and knee replacement patients from 12.5% to 2.4% in just a few years. This is much more impactful than publishing papers.”
He has also developed a senior-level course in IOE, which is IOE 413 Optimization Modeling in Healthcare. CHEPS students often take the class which is taught each fall.
Dr. Hughes is active in national service. He has been President of the American Society of Biomechanics (ASB) and is an ASB Fellow. He is also a member of the data management committee of the American Joint Replacement Registry. His work has been supported by the National Institutes of Health, Whitaker Foundation, and Blue Cross Blue Shield of Michigan/Blue Care Network.
Outside of work, Dr. Hughes is a recreational rower in the summer and skier in the winter.
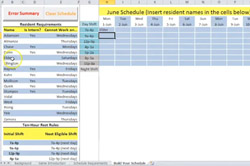
Block Scheduling
Before collaborating with CHEPS, scheduling for the residency programs at Michigan Medicine was completed by the Chief Residents entirely by hand. A daunting task, it was difficult to create high-quality schedules and was a poor use of the time of talented Chiefs who could be putting their skills to better use.
The Block Scheduling project was borne out of an already existing project in 2014. A team at CHEPS had been building the daily resident shift schedules for C.S. Mott’s Pediatric Emergency Department for several years. Over time, it was observed that most months were easy to build but some were much harder. Why? Variations in the distribution of residents assigned to the ED that month. This variability stemmed from the annual Block Schedule, and so CHEPS set out to improve this too!
The Block Scheduling team began to tackle this newly found scheduling problem by applying similar optimization techniques to those used for scheduling shifts. In the first year of the project, the team collaborated with the Pediatrics residency program to schedule their interns (first year residents) as well as with the Department of Surgery to integratively schedule for the residents and fellows across a dozen programs. In the following year, the CHEPS team expanded their work to all three years of the Pediatrics residency program and continued to build schedules for the same programs in Surgery. Currently, the CHEPS team is scheduling for Pediatrics, Internal Medicine, Combined Medicine-Pediatrics, and more than a dozen programs in the Department of Surgery. Altogether, these schedules cover more than one-third of Michigan Medicine’s physician trainees.
The current Block Scheduling team consists of Professor Amy Cohn, Associate Director of CHEPS, staff member Billy Pozehl, and students Sam Roth, Justin Steuer, Jordan Schebil, and Joseph Sorenson, from the departments of Industrial and Operations Engineering and Computer Science Engineering. They build on the work of many students and Chief Residents who have collaborated together over the years to develop these tools.
So how does the team accommodate all of these requests when creating schedules? A survey is sent out to the residents to gather all of their requests before the team tackles the scheduling. Requests can range from vacation time to when in the year a resident wishes to have a certain rotation. For this upcoming academic year, the team received an enormous number of requests. Team member Billy noted, “we have received about 2000 requests from the senior residents for this academic year’s scheduling, and we are able to satisfy the majority of them.” After the team processes the submitted requests and successfully builds a schedule, there is a meeting with the respective Chief to review their work.
Thanks to the team’s use of optimization techniques, impacted residents have been much more satisfied with their schedules. Dr. Steve Gorga, who was one of the Chiefs in Pediatrics in 2016 and is currently a fellow in Pediatric Critical Care, said of the project “I feel that the greatest benefit of working with CHEPS for block scheduling was that it gave us a known, high-quality feasible schedule that took into account all of our residents’ requests, while also giving us the ability to make tweaks later on when new and unforeseen needs arose.”
Team member Billy Pozehl, who has been with CHEPS since 2012 and is an alum of the HEPS master’s concentration, also commented on the residents’ satisfaction, “We’ve found that the residents are significantly happier with their schedules now because we are able to ensure that undesirable scheduling patterns are not given. For example, we can ensure that residents don’t get three inpatient service rotations in a row, which can burn a resident out. We can also ensure that desired vacation periods are granted or that a resident will get a particular rotation earlier in the academic year if they need letters of recommendation to do a fellowship.” Billy also noted the project’s profound impact on the hospital by saying “the schedules we create will affect over 100 different services.”
In terms of the future of Block Scheduling, the project hopes to grow into scheduling for other programs within Michigan Medicine as well as begin scheduling for other health systems. The team is busy making advances at the university’s hospital to create improved resident schedules, fully aware that there are numerous opportunities to improve the schedules of other residency programs across the country.
Recent News
- Andrea McAuliffe Awarded AAMI-HSEA Health Systems Engineering Scholarship
- Dr. Jarir Chaar Lunch and Learn
- RCA, Human Factors, & Patient Safety Workshop
- Jeremy Castaing PhD Defense
- Sung Won Choi Named Professorship
- Winter 2017 Kick-Off
- Marina Epelman, Chuck Mayo, and Dawn Owen Seminar
- Scheduling Medical Residents with Conflicting Requests for Time Off
- Mariel Lavieri, Joshua Stein, and Mark Van Oyen Seminar
- Christine Barnett and Selin Merdan Seminar
- Jim Bagian Seminar
- CHEPS Attends INFORMS
- Karandeep Singh Seminar
- Brandon Pitts Seminar
Upcoming Events
- Save the Date: 5th Annual Symposium on Healthcare Engineering and Patient Safety on Monday November 6, 2017 at 5 pm
Where in the World is CHEPS?
In this flashback “Where in the World is CHEPS,” alum Joe East, who is profiled in this issue, is pictured in Patagonia in front of Grey Glacier, the third largest glacier in the world after the North and South Polls.
See more “Where in the World is CHEPS” here.
The CHEPS Newsletter team is: Lauren Hirth (BME undergraduate student), Anna Learis (IOE undergraduate student) , Bill Zhang (HEPS masters student), Elizabeth Fisher (staff)